Bile Acid Sequestrant Interaction Checker
Check Your Medications
Enter medications you're taking. We'll check for interactions with bile acid sequestrants (colesevelam, sevelamer).
Interaction Results
When you're managing type 2 diabetes, every medication choice matters. Some drugs help lower blood sugar but cause weight gain. Others lower it well but cost hundreds a month. Then there’s bile acid sequestrants - a quiet, older class of drugs that quietly do two things at once: lower LDL cholesterol and give a modest dip in blood sugar. But they come with a price: uncomfortable side effects and tricky interactions that can make or break your treatment.
First approved for high cholesterol in the 1970s, bile acid sequestrants like colesevelam (brand name WelChol) got a second life in 2008 when the FDA approved them for type 2 diabetes. They’re not flashy. They don’t come in injectable pens. They don’t make headlines like GLP-1 agonists. But for a small group of people - especially those with both high cholesterol and diabetes - they still have a place.
How Do Bile Acid Sequestrants Work?
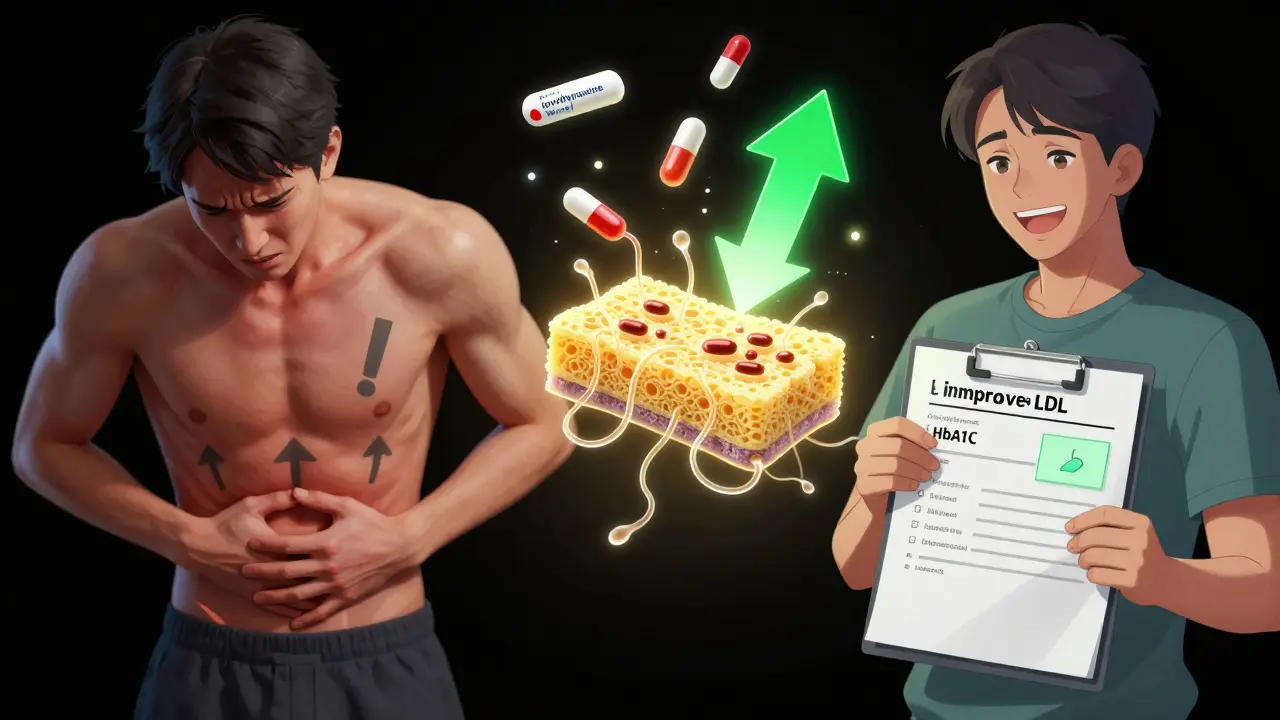
These drugs aren’t absorbed into your bloodstream. Instead, they act like sponges in your gut. Colesevelam and sevelamer bind to bile acids - substances your liver makes to help digest fat. When they’re trapped in the intestines, your liver has to pull more cholesterol from your blood to make new bile acids. That’s how LDL cholesterol drops by 15-18%.
But here’s the twist: that same process also improves blood sugar. Scientists think it’s because bile acid binding triggers signals in your gut and liver that improve how your body handles glucose. It’s not fully understood, but studies show this effect is real. On average, colesevelam lowers HbA1c by about 0.5%. That’s not huge - metformin drops it by 1-2%, and newer drugs like semaglutide can drop it by 1.5% or more - but for some people, even a half-point drop matters.
The Side Effects You Can’t Ignore
If you’ve ever taken a chalky powder mixed with water, you know what we’re talking about. Colesevelam comes as tablets you swallow with meals. But it’s gritty. It’s thick. And it doesn’t dissolve well.
That’s why gastrointestinal side effects are so common. About 1 in 3 people report constipation. Nearly 1 in 4 say they feel nauseous. Bloating and gas? That’s another 1 in 5. In clinical trials, about 19% of people stopped taking colesevelam because of these symptoms. That’s nearly four times the rate of placebo.
Real-world reviews tell the same story. On Drugs.com, over 49% of users rate it as “poor.” One Reddit user wrote: “I needed Miralax just to go to the bathroom.” Another said: “It felt like swallowing sawdust. I couldn’t keep it down.”
And it’s not just discomfort. In rare cases, it can lead to serious problems. There are documented cases of bowel obstruction - especially in people who don’t drink enough water or already have slow digestion. One patient described being hospitalized after three months of use. The drug doesn’t cause this often, but when it does, it’s dangerous.
Drug Interactions: A Hidden Risk
This is where bile acid sequestrants get really tricky. Because they stick to everything in your gut - not just bile acids - they can also bind to other medications and stop them from working.
The FDA says you must take other drugs at least 4 hours before or 1 hour after colesevelam. That’s not easy to manage. Imagine trying to fit this schedule around breakfast, lunch, dinner, and your other pills. It’s a logistical nightmare.
Here are the most common and dangerous interactions:
- Thyroid hormones (levothyroxine): If you take this for hypothyroidism, colesevelam can cut its absorption by up to 50%. That means your TSH could rise, and you’d feel tired, cold, and gain weight - even if you’re taking your dose.
- Warfarin: This blood thinner’s effectiveness depends on consistent absorption. If colesevelam interferes, your INR could swing dangerously. One study found patients needed more frequent blood tests after starting the drug.
- Sulfonylureas (like glipizide): These older diabetes pills can lose effectiveness. You might think your diabetes is worsening, when it’s just the drug interaction.
- Metformin: Even though both are often used together, colesevelam can reduce metformin absorption by up to 10%. That’s not enough to stop it from working, but it’s enough to make your doctor wonder why your A1c isn’t dropping.
- Statins (simvastatin, atorvastatin): Colesevelam cuts simvastatin levels by 40% and atorvastatin by 20%. If you’re on both, your cholesterol might not go down as expected.
Doctors have to check every medication you take - not just diabetes drugs. Many patients don’t realize this. A 2015 study found that nearly 60% of patients on colesevelam were also taking at least one interacting drug, and only 32% were given proper timing instructions.
Who Actually Benefits?
For most people with diabetes, bile acid sequestrants aren’t the best choice. But for a specific group, they make sense.
Think about someone who:
- Has type 2 diabetes with an HbA1c around 7-8%
- Has high LDL cholesterol (above 130 mg/dL)
- Can’t take statins because of muscle pain or liver issues
- Is already on metformin but needs extra help
- Wants to avoid injections or weight-loss drugs
That’s the sweet spot. These drugs don’t cause weight gain or low blood sugar - two big downsides of other options. And for people who can’t tolerate statins, getting both cholesterol and glucose control from one pill is a rare win.
One patient on Drugs.com wrote: “My LDL dropped from 142 to 98. My A1c went from 7.1 to 6.8. I still have constipation, but it’s worth it.” That’s the kind of trade-off that makes sense - if you can handle it.
The Decline of Bile Acid Sequestrants
Once a popular option, these drugs are fading fast. In 2012, over 1.7 million prescriptions were filled for colesevelam in the U.S. By 2023, that number dropped to under 900,000. Today, it makes up less than 0.5% of all diabetes prescriptions.
Why? Because newer drugs do more. GLP-1 agonists like semaglutide don’t just lower blood sugar - they help you lose weight, protect your heart, and reduce your risk of kidney disease. SGLT2 inhibitors do the same. Both have proven benefits in large trials. Bile acid sequestrants? They’ve never shown a reduction in heart attacks or death.
Even the American Diabetes Association says they’re not first-line. The American Association of Clinical Endocrinologists calls them a “third-line option.” And in Europe, regulators haven’t approved any for diabetes at all.
Pharmaceutical companies have mostly given up. Genzyme stopped trials for sevelamer in diabetes in 2021. No major drugmaker is investing in new bile acid sequestrants - except for one experimental version (Elobixibat analog) with fewer side effects. But even that’s still in early testing.

Practical Tips for Taking Them
If your doctor prescribes colesevelam, here’s how to make it work:
- Start low. Begin with 1,875 mg per day (three 625 mg tablets). Increase slowly over 2-4 weeks. This helps your gut adjust.
- Take with meals. Always take it with food. It helps with absorption and reduces nausea.
- Drink water. Aim for at least 8 glasses a day. Fiber helps too - oats, beans, apples. But don’t overload fiber right away; it can make bloating worse.
- Time other meds. Separate other pills by 4 hours before or 1 hour after. Set phone alarms. Write it on your calendar.
- Watch for signs of trouble. If you haven’t had a bowel movement in 3 days, or feel bloated and painful, call your doctor. Don’t wait.
- Check your other meds. Bring a full list of everything you take - including vitamins and supplements - to every appointment.
Adherence is low. Only about 65% of people stick with it after six months. But if you can get through the first month, many find the side effects ease up. And if your cholesterol and blood sugar improve? That’s a win.
What’s Next?
Bile acid sequestrants aren’t going away - but their role is shrinking. They’re not for everyone. They’re not for most people. But for a small group - older adults with diabetes and high cholesterol who can’t take statins - they still offer a rare combo benefit.
The future may lie in combining them with newer drugs. Early trials are testing colesevelam with semaglutide. The idea? Use the bile acid effect to boost GLP-1 action, while reducing the side effects of both. It’s promising, but years away from real-world use.
For now, if you’re considering this drug, ask yourself: Is the cholesterol benefit worth the daily discomfort? Can you manage the timing of your other meds? Are you prepared for the possibility that it might not even help your blood sugar much?
There’s no shame in choosing something simple. But you need to know the trade-offs - before you start.





Write a comment
Your email address will be restricted to us